Covid-19 community response: The case of South Asians in Auckland, New Zealand
Capacity building and community cohesion are essential to prepare the population for a possible future re-emergence of the pandemic outbreak

Global statistics and research on mortality risk of Covid-19 indicate that ethnic minorities worldwide are more vulnerable to the novel coronavirus. Multiple factors affect the higher mortality risk for ethnic minorities, characterising socio- economic hindrance, a greater burden of chronic diseases, and poorer access to healthcare services.
The Covid-19 pandemic has been everything but the great equaliser. It, on the contrary, seems to deepen inequality and intensify racism. Ethnicity-associated inequality and racism have a significant gradient in health outcomes.
These factors are expected to play a negative role in the wellbeing of minority ethnic groups in New Zealand. One of the key ethnic groups in New Zealand is the Asian ethnic group, which is the third-largest group (15.1% of the population) based on Stats NZ 2018 census. According to the census, Indians (4.7%), Chinese (4.9%) and Filipinos (1.5%) are the largest groups. The remaining 4% belong to all other countries within Asian ethnicity.
Other South Asian populations (i.e. Afghanistan, Bangladesh, Bhutan, the Maldives, Nepal, Pakistan, and Sri Lanka) make up less than 1% each of the nation's population according to census 2013. The South Asian ethnic group is considered the "model minority" and the fastest-growing minority group in New Zealand.
It is characterised by cultural diversity and a high level of engagement in small family businesses, such as restaurants, and grocery and boutique shops. This population is considered to have a higher vulnerability to pandemic-related risks.
It is speculated that South Asians overseas showed higher burden of comorbidities and susceptibilities, though they were considered comparatively healthy based on causal knowledge, e.g. lower rate of smoking and alcoholism, a higher rate of vegetarianism, and lower body mass index (BMI).
Health presentations of different ethnic groups varied due to physiological divergences. Even South Asian sub-groups have a wide variety of heterogenicity. Health presentations of this ethnic group often puzzle researchers, and it has not yet led to a theory to be accepted widely.
New Zealand's Ministry of Health reported that Asians are the second-highest infected group (15%, 236 cases as of 9am local time on August 15). Of them, the total number of South Asians is not well-defined. Thus, more research and granular ethnicity data are essential for health emergency response and community resilience.
This policy brief is based on the survey of the South Asian community living in New Zealand and their coping with the Covid-19 impact. The findings of this survey may also be useful for other ethnic groups. Understanding the impact of a pandemic on ethnic minority groups is important to better prepare for transition and recovery strategies, and build community resilience.
Data collection and analysis
We conducted a cross-sectional survey utilising a semi-qualitative method to collect and analyse data about the South Asian population's socioeconomic, health and wellbeing status during the Covid-19 pandemic restrictions.
The questionnaire was designed to gather responses on a scale from 1 to 10 to enable ranking (in percentage) within the South Asian ethnic group. We focused on obtaining information on stress level: (i) age, ethnicity, income and residency status, (ii) social and personal wellbeing impacted by Covid-19 restrictions, (iii) health accessibility and physical wellbeing impact due to lockdown, and (iv) stress and psychological wellbeing.
A self-administered online survey was conducted using Survey Monkey from April 20 to May 30, 2020. The link was shared in various social media platforms. OpenEpi was used for power calculation of the sample size, and we considered the targeted population as a representative sample of the community. Compared to a large population, the total number of responders is limited and only reflects an indicative overview or partial facts of this study.
Due to its nature (i.e., online survey), this survey did not include those who are not online survey friendly, and disabled, aged, and the disadvantaged population who do not have access to the internet. Incidentally, these people are also considered to be the most vulnerable to the pandemic effects. A more comprehensive mixed-method (i.e., both household and online surveys) may be conducted in future to capture these groups.

Results from 65 out of 87 respondents were analysed. Participants who reported ethnicity as the Philippines, Europe or unknown country were excluded from the dataset. Data were analysed based on clusters, ethnicity, and age groups to understand the overall stress level.
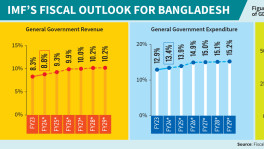
Indian and Bangladeshi communities reported the highest levels of stress within South Asian communities, with a relative frequency of 32.6% and 23.5% respectively. The Sri Lankan community reported lower levels of stress (5.1%) (Figure 1).
The government of New Zealand introduced wage subsidy payment to support employers, including self-employed people, who were significantly impacted by Covid-19. Regardless, the stress related with income and employment within the South Asian ethnicity was substantial (Figure 2).

It has been recognised that economic impacts of Covid-19 restrictions have been especially devastating for small businesses, also indirectly affecting social and personal wellbeing through mental health consequences. The South Asian community has, therefore, been highly affected, given their engagement in small family businesses.
The stress during Covid-19 lockdown was equally high across the South Asian community. Indian and Pakistani responders mentioned that their income reduction was up to 41% from the regular income.
In terms of age groups, those in the 40-59 age group were highly stressed across the whole ethnic community (Figure 3). However, stress level varies for different clusters for age groups. 18-39 age group mostly suffered from employment and income situation, 40-59 age group had prolonged stress on income, employment and personal wellbeing, and 60-79 age group had a similar prolonged stressed situation (Figure 4).
Community-level policy recommendations
Three days after the World Health Organisation declared the coronavirus outbreak a public health emergency of international concern on January 30 this year, New Zealand began introducing disease prevention measures. It took early and hard action.
The country's strategy was based on speedy testing, contact tracing and isolation (lockdown), while rigorously adhering to public health guidance. New Zealanders were in lockdown for 74 days. The decision to introduce lockdown only after 100 cases proved to be a key one in the fight against Covid-19.
At the time of writing this policy brief (mid-August 2020), New Zealand is facing the second wave of Covid-19. Nationally, it is well-prepared for second and possible future pandemic responses.
However, looking at the nature of second waves (e.g., in Victoria, Australia) and from the findings of this survey, it seems that at the community level, we are not understanding the pandemic consequences and are not well-prepared for coping with pandemic events.
Capacity building and community cohesion are therefore essential to prepare the population for a possible future re-emergence of the pandemic outbreak. Some policy recommendations include:
• Develop a well-functioning data ecosystem to understand outbreak and transmission for ethnicities: The Ministry of Health currently disaggregated ethnicity in five major categories (Māori, Pacific, Asian, other and unknown) and that is insufficient to look at the more granular situation within the community level. As a diverse community, South Asians should be sub-divided based on the given shreds of evidence. Different ethnicity within Asia varies with culture and health contexts.
Strengthening capacity to understand transmission, outbreak assessment, risk communication, and cascading impacts assessment on essential and other services is crucial. The use of data from people is becoming strictly controlled, whereas contact tracing is required to comprehend the disease transmission. A data ecosystem is critical to ensure a stable transition from response to the recovery phase.
• Research and innovative programme: More systematic research with homogeneous clusters or small minority groups is recommended to better comprehend the health and social data during pandemic. Amalgamating the whole Asian ethnicity would misguide both health professionals and the community. Extensive health research would allow New Zealand to be more resilient to respond to pandemic and other cascading and compounding risks.
• Invest adequately in culture-based community preparedness: Community-level preparedness and contingency plan for identifying suspected cases, isolating and/or quarantining them, accessing health services, and arranging employment or financial support could be prioritised. Each minority group has a unique culture (e.g. Māori). Adopting their own culture and context would enhance community trust and empowerment.
The authors work at the University of Auckland.


 Keep updated, follow The Business Standard's Google news channel
Keep updated, follow The Business Standard's Google news channel