Biomedical waste amid Covid-19 put public environmental health at risk
Bangladesh was already struggling with poor medical waste management before the Covid-19 pandemic and has now been hit hard by a sudden increase in the volume of medical waste

Biomedical waste is a threat to global public environmental health, especially in the lower-middle-income countries such as Bangladesh. Worldwide, it is estimated that at least 5·2 million people, including 4 million children, die each year because of diseases related to unmanaged medical waste.1 Considering the transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) globally, excessive biomedical waste has become a new major threat to public health and the environment. Improper handling of hospital waste might aggravate the spread of SARS-CoV-2 to medical staff and people who handle waste.2
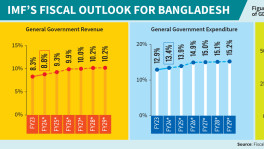
Bangladesh was already struggling with poor medical waste management before the Covid-19 pandemic and has now been hit hard by a sudden increase in the volume of medical waste. In Bangladesh, there are around 654 government hospitals and 5055 private hospitals and clinics with 141 903 beds in total, along with an additional 9061 diagnostic centre beds, all of which lead to the generation of huge amounts of biomedical waste. The average medical waste generation rate is 1·63–1·99 kg per bed per day in Dhaka, the capital of Bangladesh.3 In April 2020, at least 14 500 tonnes of waste from health care was generated across the country because of Covid-19,4 which has undoubtedly increased due to the increasing infection rate. Also, on average, 206 tonnes of medical waste are produced because of Covid-19 per day in Dhaka alone.5 This poorly managed waste poses a large environmental threat and might create a prolonged and unwanted public health hazard and be a potential source of re-emerging infection.
In Bangladesh, despite the introduction of the Medical Waste Management and Processing Rules in 2008, no safe system has yet been developed to manage the health-care waste generated daily in hospitals, clinics, and households. Waste generated inside Bangladeshi hospitals is often collected without any separation by untrained, unprotected, and unaware cleaners, and disposed of in unauthorised places without any separation or proper treatment.6 Approximately 40 000 informal waste collectors working across the country are at high risk of getting infected by SARS-CoV-2 because they work without adequate protection.7 There might be a serious risk of spreading SARS-CoV-2 if used masks, gloves, and other personal protective equipment are not managed and disposed of properly. Additionally, household waste (eg, tissues, masks, gloves) puts waste management workers at increased health risk.
In Bangladesh, hospital waste is mainly managed by city corporations, third-party organisations, and non-governmental organisations. However, the capacities of these stakeholders do not comply with the requirements of a proper, environmentally safe medical waste disposal mechanism. A policy-level paradigm shift into a strategic, state-of-the-art medical waste management system is required. Failing to tackle the huge surge in medical waste amid Covid-19 is likely to put Bangladesh at further environmental and public health risk.
This article, written by Md Mostafizur Rahman, Md Bodrud-Doza, Mark D Griffiths and Mohammed A Mamun, was first published in The Lancet Global Health on August 13.


 Keep updated, follow The Business Standard's Google news channel
Keep updated, follow The Business Standard's Google news channel